Johns Hopkins Plans 60 Penis Transplants for Injured Veterans
A promising new surgical technique for male genitalia.
With almost daily technological developments in sex tech, it’s important not to overlook innovations that are not hardware or software—but rather exist in the very intimate world of medicine.
 |
Case in point: doctors Gerald Brandacher, W.P. Andrew Lee, and Richard J. Redett at the prestigious Johns Hopkins University School of Medicine in Baltimore are planning the first-ever penis transplant in the United States. It will be conducted in perhaps only a few months.
The operation will be performed on a wounded Afghanistan war veteran and, if all goes well, the patient should be able to have urinary function, feeling, and even the ability to eventually function sexually. Though doctors caution that total restoration, such as having the ability to father children, is unlikely at this time.
To date, two other attempts at penis transplants have taken place—with mixed results. The first was performed in 2006 in China and, unfortunately, was not a success.
However, another attempt in 2014 by professors Frank Graewe, André van der Merwe, and Rafique Moosa in Tygerberg Hospital, South Africa, did succeed—leading to the current project by Johns Hopkins.
Initially, the focus for the first attempt in the United States as well as plans for future transplants will be wounded soldiers.
Chairman of Plastic and Reconstructive Surgery at Johns Hopkins, Dr. W. P. Andrew Lee, said to The New York Times, “I think one would agree it is as devastating as anything that our wounded warriors suffer, for a young man to come home in his early 20s with the pelvic area completely destroyed.”
There are already discussions underway that, if the first operation meets all of the doctor and patient’s expectations, that it may be adapted for gender reassignment surgery.
Johns Hopkins bioethicist Jeffrey Kahn, speaking at the Intimacy After Injury Conference in 2014, said, “Once this becomes public and there’s some sense that this is successful and a good therapy, there will be all sorts of questions about whether you will do it for gender reassignment.”
The surgery
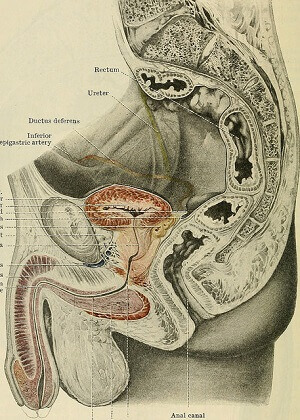
The operation itself is planned to take approximately 12 hours, involving connecting as many as six nerves, and seven arteries and veins using microsurgical techniques.
Previously, plastic surgery has been able to give patients a somewhat accurate version of a penis mostly involving skin grafts. But these techniques don’t offer many of the basic functions of a real sexual organ, most importantly sexual sensation.
Yet, while there is hope that penile transplant patients will regain much of their previous sexual lives, a transplant raises a few unique issues—not least of which being psychological.
Issues and concerns
On the donor’s side, one concern is how to approach the relatives of the deceased. Few organs, after all, carry with them such intimate significance as genitalia. This is an especially sensitive area as, for the transplant to be successful, it is preferable that the donor is healthy and young at the time of his passing.
The other emotional concern is from the person receiving the transplant. However, many have said that the benefit of being able to even partially restore sexual function will more than likely override any patient concerns.
Dr. Gerald Brandacher of the Johns Hopkins surgical team compared the penis transplant to his experiences with patients having undergone hand replacement surgery.
“I can tell you from all the patients—and I’ve been involved since 1998—every single one, after surgery, look at the graft, try to move it and they immediately call it ‘my hand.’ They immediately incorporate it as part of their body. I would assume, extrapolating, that this is going to be the same for this kind of transplant,” he said to The New York Times.
While this penis transplant procedure is untried, Johns Hopkins has given permission for the surgical team to conduct 60 of the operations this year if the initial trial is successful.
If all goes well, soon transplanting penises—and perhaps other human sexual/sensual organs—will be commonplace enough to both heal those who have suffered physical and emotional injuries and also provide an opportunity for others to become their true sexual selves.
Image source: Internet Archive Book Images, Johns Hopkins Medicine
Leave a reply
You must be logged in to post a comment.