First U.S. Womb Transplant May Allow Infertile Woman to Give Birth
Trans women and men could one day become pregnant, too.
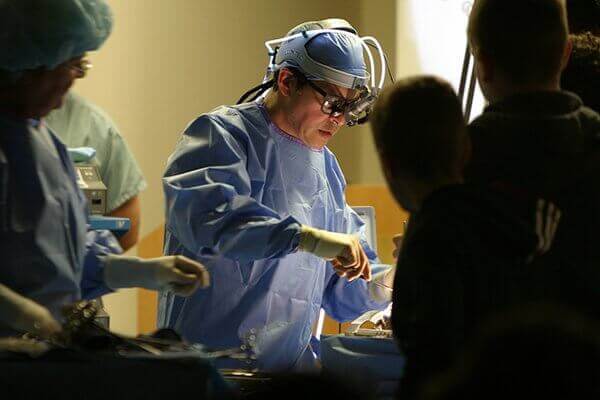
Surgeons at the Cleveland Clinic have become the first in the United States to perform a uterus transplant. The nine-hour surgery took place on Feb. 24 when an organ from a deceased donor was successfully implanted into a 26-year-old patient.
If the trial’s success continues, it may give women born without a uterus, or who have had one removed due to uterine damage, their only chance to carry a child. This transplant is one of ten test procedures planned by the clinic.
How the experimental transplant works
The uterus, cervix, and part of the vagina are removed from the donor. Surgeons also remove the small blood vessels that are connected to the uterus. These vessels then connect the donor’s uterus to the patient’s larger blood vessels on the outside of the pelvis. If the patient still has fallopian tubes or ovaries, they are left unconnected.
Because of the nature of the transplant, it’s impossible for recipients to give birth naturally. They will have to wait a year after the procedure for their bodies to heal before starting in vitro fertilization (IVF). When ready, the baby is delivered via caesarean.
Like all transplants, the patient is required to take anti-rejection medication. Because of this, the uterus is removed after one or two babies have been born.
But there are downsides and concerns
In addition to the Cleveland Clinic, other organizations around the world have begun their own trials. However, naturally, the transplant raises a number of medical and ethical concerns. Despite the eagerness shown by potential candidates, some argue that high-risk procedures should only be performed when attempting to save lives.
The use of anti-rejection drugs poses potential difficulties as well. It’s still unclear how they may affect a developing fetus. The known side effects include increased risk of infection and possible preterm delivery. However, several women who became pregnant while taking the drugs for a kidney transplant experienced no serious side effects.
Unlike previous trials, both the Cleveland Clinic and Womb Transplant U.K. are using organs from deceased donors. Although this is beneficial in excluding risk to healthy donors, the effects are unknown, adding to the many possible pitfalls of such an experimental process.
The procedure is at the forefront of medical innovation. Previously, Sweden’s University of Gothenburg had been the only group to have successfully performed the transplant to result in births. Nine women received uteri from live donors, resulting in five pregnancies and four births. All of the babies were born prematurely, but otherwise healthy.
Benefits may extend to trans women and men
It’s taken the Cleveland Clinic over a year to develop a plan that meets safety approval, and a lot of their knowledge has come from the results of the University of Gothenburg, as well as failed attempts abroad. The clinic’s recent patient was one of ten women being screened for the procedure. A 26-year-old candidate told the New York Times that despite having two adopted children, she still craves the chance to become pregnant and give birth.
“I want the morning sickness, the backaches, the feet swelling. I want to feel the baby move. That is something I’ve wanted for as long as I can remember.”
It’s possible that this transplant technology could allow more than just cis women born physiologically female to carry a child. According to Karine Chung, director of the fertility preservation program at the University of South Carolina, transgender women may have the opportunity to carry their own children in the next five to ten years.
There are, however, several issues that need to be worked through. Currently, the transfer of the embryo into the uterus is done via the vagina and cervix. For trans women, this would mean implanting a constructed vagina to attach to the uterus, which has never been attempted.
The use of synthetic hormones also raises concerns. Justine Evans from Creation Fertility, who specializes in IVF treatment, told The Huffington Post the amount of drugs needed to maintain the pregnancy could prove problematic to the health of both mother and child, as well as future generations. Additionally, the process would be costly, ruling out many potential candidates.
But there is hope. While options for trans couples to foster and adopt remain limited, the possibility of extending uterine transplants to cater to their needs has been named theoretically possible by the Cleveland Clinic. This means that, in time, it may be regular for both trans and cis women, as well as men, to carry children.
The Cleveland Clinic’s recent transplant provides an immense opportunity. If future trials are successful, there are an estimated 50,000 potential U.S. patients who could benefit. And as we continue to trial and learn, we may make motherhood a reality for those it had previously been considered impossible.
Medically, the future of motherhood may be limitless. The path to making that possible lies in our attitudes and acceptance towards those wanting to give birth to a child.
Image source: Eric Schmuttenmaer
Leave a reply
You must be logged in to post a comment.